COVID-19 is on rise in SLO County. What’s behind the summer surge?
As temperatures have risen across San Luis Obispo County, new cases of COVID-19 are on the rise, too.
Though the 2020 outbreak of the COVID-19 pandemic is now five years in the rearview mirror, neither time nor a decline in the public’s level of interest in stopping the disease’s spread have changed the fact that new variants of the illness are still impacting people this summer.
San Luis Obispo County deputy health officer Dr. Rick Rosen said the latest surge in COVID-19 infections lines up with the trends established in more recent years of the pandemic: slower rates of spread in the spring and fall and larger spikes around summer and the winter holidays.
Despite the higher number of infections, COVID-19 fatalities have generally declined since the start of 2022.
According to the Centers for Disease Control’s weekly report on U.S. COVID-19 fatalities, just 123 deaths were reported as being caused by COVID-19 in the week of Aug. 23. The number of deaths has been on the decline since January, when more than 1,000 people died in the weeks of Jan. 4 and Jan. 11.
Still, that only tells part of the story, Rosen said.
While deaths related to COVID-19 have been on the decline for years, the illness is still spreading quickly in some of the most vulnerable communities, including older adults, immunocompromised individuals, individuals living with chronic heart and lung diseases and other vulnerable populations, Rosen said.
“It is pretty clear to us at the Public Health Department that COVID activity and COVID transmission is up locally — it’s also the case that COVID transmission is up across the state of California, and our local numbers and the state are tracking pretty closely,” Rosen said. “In addition to wastewater, we’ve seen increased activity in what we call high-risk congregate settings like assisted living facilities, homeless shelters and correctional facilities.”
COVID-19 surge sweeps country, but fatalities are few
Based on the most recent COVID-19 wastewater detection and test positivity data made available by the county, cases of COVID-19 in San Luis Obispo County have been on the rise since the start of the summer, though not to the same extent as previous spikes.
Wastewater detection data posted by the county doesn’t measure specific amounts of diseases like COVID-19 in the wastewater, but does provide a good picture of how COVID-19 detection compares to previous spikes, Rosen said.
“Because the methodology for wastewater sampling and reporting varies depending on the lab that is performing the analysis, our epidemiology team does not share the units in the graphs,” Rosen said in an email. “It is similar to the concept that the state uses with its low/medium/high reporting.”
According to the county’s health dashboard, wastewater detection levels in the summer of 2025 are currently tracking slightly higher than they were in January, following several months of lower detection levels in the spring months. While detection levels from this summer are higher than they were at the start of the year, they’re also lower than they were this time last year.
Detection levels in San Luis Obispo and Cambria were generally lower than the rest of the county, with detection levels mirroring those of January, while wastewater systems in Paso Robles, Atascadero, Los Osos and South County showed signs of COVID-19 levels closer approaching the levels from last summer.
Test positivity — a metric that measures the number of positive results for a given virus divided by the total number of tests performed — shows a similar trend for COVID-19 across the county, with this summer showing similar numbers to the summer of 2024.
In both time spans, COVID-19 test positivity in PCR or professional antigen tests consistently reached above 50%, according to the county dashboard.
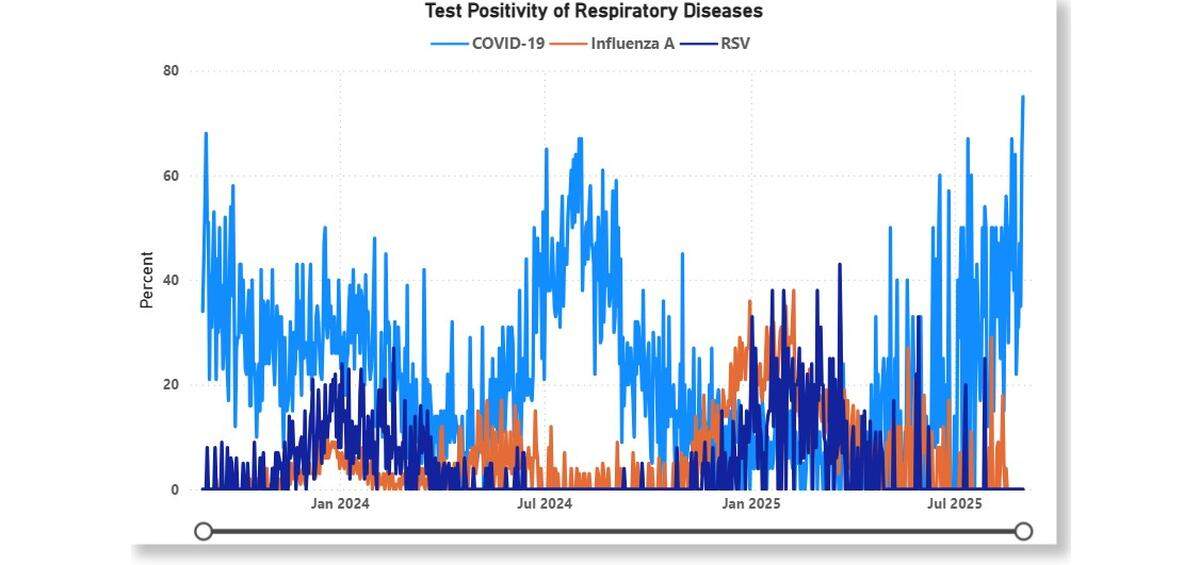
Currently, the predominant COVID-19 variant that people are being infected with is known as the “XFG” variant, which isn’t associated with an increase in severity of the disease, Rosen said.
Though its lethality is lower than previous strains, Rosen said it’s still in the best interest of vulnerable people — and the people around them — to exercise caution and use personal protective equipment.
Rosen said around 10% of adults who have a mild COVID-19 infection will develop long COVID — a chronic version of the illness that can persist for weeks to years following an initial infection — while a quarter of adults who experience a severe initial infection can develop long COVID.

Hospitals seeing fewer hospitalizations from COVID-19
Adventist Health Sierra Vista emergency medicine chair Kathryn Haran said with the advent of at-home testing and the end of COVID-19-related mandates on social distancing and masking, tracking the disease’s spread has become less reliable.
While it’s become less common for patients to come to the emergency room specifically seeking help for COVID-19 symptoms, it’s still relatively common to find COVID-19 in patients presenting with respiratory symptoms, Haran said.
In 2025 so far, around 13% of patients tested for respiratory illness at Adventist Health’s Sierra Vista hospital tested positive for COVID-19, while at Twin Cities hospital, that same figure was around 22%, she said.
“I usually call it ‘COVID and’ — it’s COVID and something else that’s making them require hospitalization,” Haran said. “COVID alone, we’re not seeing as many people hospitalized, and hopefully that’s due to a lot of people having at least one or multiple COVID vaccines as well.”
Because Sierra Vista no longer tests all incoming patients — emergency room or otherwise — for COVID-19, only patients exhibiting respiratory illnesses are tested, so the number of people with COVID at the hospital may be higher, Haran said.
“Typically, we have the winter surges with respiratory viruses like RSV and influenza and things like that, that peak in the winter time, so the summer spread is definitely new with COVID,” Haran said. “I think the transmissibility of COVID, where it’s easily contracted with summer travel, being on airplanes, visiting family from other states — it just allows for a lot more mixing of this virus and transmission between people as they travel for the summer.”
Currently, only two patients at each of Adventist Health’s hospitals are under the hospital’s care specifically for COVID-19, which is relatively normal, according to Adventist Health business development executive Shannon Downing.
Rosen said as the pandemic has progressed, San Luis Obispo County has been lucky to avoid spikes in infections requiring hospitalizations, meaning hospitals haven’t had to deal with as much strain on their bed capacity due to COVID-19 as they have in the earlier years of the pandemic.
Still, staying vigilant for those at the highest risk remains a priority for health officials, he said.
“We at the Public Health Department stay in touch with high-risk congregate settings around the county,” Rosen said. “We continue to make personal protective equipment like surgical masks and N95s, eye protection, gowns and gloves available in those settings, and our goal is to continue to do that through the end of this calendar year.”