SLO nurse lost her baby after delivery. Now, she’s buying CuddleCots to help others
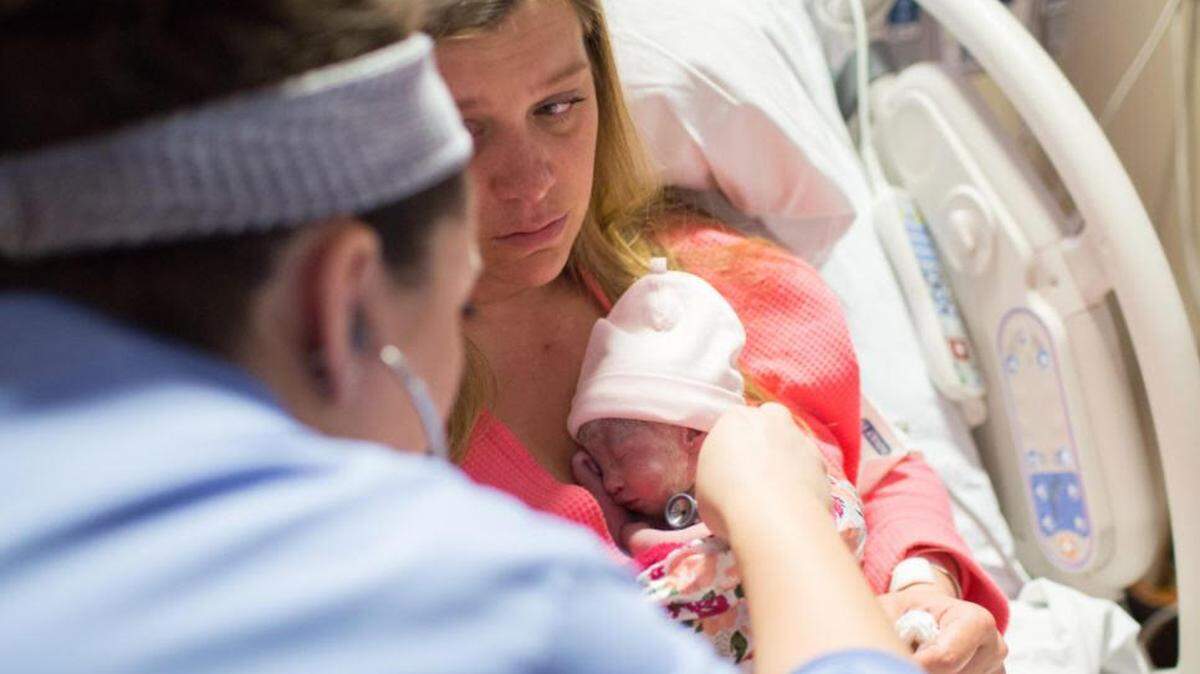
Ashley Agnitch was about 12 weeks pregnant in 2017 when she received heartbreaking news.
The baby she was carrying had Trisomy 18, a rare genetic condition that made it unlikely the infant would survive pregnancy, labor and delivery.
“Babies with Trisomy 18 are considered incompatible with life,” said Agnitch, a labor and delivery nurse at French Hospital Regional Medical Center who lives in Arroyo Grande.
Because the only outcome for babies born with Trisomy 18 is death, some families with this diagnosis choose to terminate the pregnancy. Although doctors offered the Agnitch family this option, they decided to continue the pregnancy.
“That was our own personal choice,” Agnitch said. “We wanted to give her whatever life we felt she could have, and show her love and try to celebrate whatever moments we did have (with) her in our lives.”
The delivery revealed to Agnitch a gap in care that could have helped ease the pain of a heartbreaking experience.
If she had had access to a special cooling bassinet called a CuddleCot, she could have extended the time she and her family had to bond with and grieve for the baby they named Greta.
Now, she’s doing something about it to help future mothers in the same situation.
“I did not get (a CuddleCot) for Greta and always feel that it would have made a huge difference,” she said.
How CuddleCot could have improved family’s delivery experience
Most pregnancies with Trisomy 18, also called Edwards Syndrome, end in miscarriage or stillbirth. A third of Trisomy 18 babies are born premature, and more than 40% die in labor, according to the Cleveland Clinic.
The condition occurs in every 1 in 6,000 to 1 in 8,000 live births, according to Boston Children’s Hospital.
The life expectancy for fetuses with Trisomy 18 and babies born with the condition dwindles with time.
But as Agnitch’s pregnancy continued to progress, the family had to prepare for their second child’s possible life as well as her inevitable death.
The family set up a crib in the nursery, they bought a couple of preemie outfits, and they waited.
Despite the slim odds, Agnitch was able to carry her baby to term and on April 12, 2017, she gave birth to her second daughter, Greta Lynn Agnitch at French Hospital.
Before her birth, Agnitch advocated for infant palliative care, so her daughter’s pain was eased to make her comfortable before she died, she said.
“I’m not going to sit here and watch my newborn baby suffer and die,” Agnitch said. “I want to know she’s comfortable.”
Greta survived about five hours, and in life was surrounded by family and friends.
Despite the grief, the family experienced joy as well. They brought her a birthday hat, as is their tradition for children on their day of birth, she said. There was laughter along with tears.
“Of course, I don’t have any regrets,” Agnitch said, as she reflected back on Greta’s life and death. ”We were just so proud that she was our baby.”
However, if the family had been given access to a CuddleCot, they would have had more time to process an experience that blends birth and death, hello and goodbye in a fleeting period of only a few hours, Agnitch said.
In memory of Greta, Agnitch recently launched a fundraiser to purchase CuddleCots for local hospitals to help families cope with infant loss.

CuddleCots come to three Central Coast hospitals
In November 2021, Agnitch started a GoFundMe page dedicated to purchasing CuddleCots for hospitals on the Central Coast.
As of Feb. 22, she has raised $12,950, enough to buy CuddleCots for the birthing centers at three local hospitals but still short of her $16,000 fundraising goal.
Two CuddleCots went to the birthing centers at the Dignity Health affiliates: one to Marian Regional Medical Center in Santa Maria and another to French Hospital Medical Center in San Luis Obispo, according to a news release from Dignity Health Central Coast.
When an infant dies at Sierra Vista Regional Medical Center, which is managed by Tenet Health Central Coast, the staff uses cooling blankets from the neonatal intensive care unit (NICU) to give families every moment possible before the baby has to be taken to the morgue, said Emily Hosford, clinical manager of Women and Children’s Services at Sierra Vista.
“We do everything we can to support families in spending as much time as possible with their baby, such as helping with photography time or baths. We also create a ‘memory box’ for the family that could include the baby’s footprint, the baby’s name card, the blanket in which the baby was swaddled, a snippet of hair, and even the tape that measured the baby’s length at birth,” Hosford said.
Last month, Agnitch ordered a CuddleCot for the birthing center at Sierra Vista, which is run by Tenet Health Central Coast, she said.
“Adding this technology to our support is another important way that we can give a family precious, irreplaceable time and memories,” Hosford said. “This is something that not only helps families in distress, it can have a positive impact on staff that has been going through so much these past couple of years.”
CuddleCot gives grieving families time for a slower goodbye
When a baby dies or is born dead, families only have a brief time before the infant’s appearance begins to change, Agnitch said.
“The process of death occurs really rapidly in infants, so your time to handle your baby is actually very short,” Agnitch said.
Since Greta was born alive and at full-term, the family had some time to hold her, wrap her and be with her in her five hours of life.
It was important to the Agnitch family that they take a family photo that included their first child, Dempsey Agnitch, who was a toddler when Greta was born.
Even though it was way past her bedtime, Dempsey came to the hospital to meet Greta and get some photos while the baby was still alive, Agnitch said.
The family also hired a photographer, Ashley Christine, who captured Greta’s life and death with care and sensitivity. She has since become a close friend of the family, Agnitch said.
These photos are what the family uses to tell their story, remember Greta and now to raise funds to bring CuddleCots to grieving families, Agnitch said.

“Once they start changing, you don’t necessarily want to remember them that way. So you’re kind of done,” Agnitch said. “Whereas the CuddleCot, it really preserves the way the babies look.”
The CuddleCot was created by Flexmort, a United Kingdom-based mortuary sciences company. The device includes a Moses-style bassinet and special pad that keeps the infant’s body cool.
“It’s still cooling, but it’s all disguised in this little bassinet that looks cute, like any other little bassinet,” Agnitch said. “It stays right by the bedside. It’s very quiet. It doesn’t sound like a refrigerator or something.”
If the Agnitch family had access to a CuddleCot, they would have been able to take more photographs with Greta and Dempsey while still preserving her appearance, Agnitch said.
“The parents have more opportunity to handle them, to bond with them, to just reach over and put their hand on them,” Agnitch said. “It creates the opportunity to not have them separated, and to really take their time.”
Infant deaths are not uncommon but are often sudden and unforeseen
While the genetic condition that caused Greta’s death is rare, many other situations can lead to pregnancy loss and infant death in the United States.
For many families, the death of a newborn is unexpected.
Miscarriages are common, particularly in the first trimester, or before 12 weeks of gestation. Roughly 10% to 15% of known pregnancies end in miscarriages, according to the March of Dimes.
The window narrows in the second trimester, between 13 and 19 weeks of gestation, when about 1% to 5% of pregnancies end in miscarriage, the March of Dimes said.
While pregnancy loss before 20 weeks of gestation is classified as a miscarriage, preterm birth refers to any baby born before 37 completed weeks of gestation, according to the World Health Organization.
Preterm birth is commonly associated with infant death. Complications stemming from prematurity are the leading cause of death among children worldwide, according to the WHO.
In the United States, the preterm birth rate has increased steadily from 9.57% in 2014 to about 10.09% today, according to the Centers for Disease Control and Prevention (CDC).
“Most of the time, people don’t know this is their outcome, so they don’t have all these decisions made ahead of time,” Agnitch said. “So they’re scrambling.”

The CuddleCot allows families to take time to bond with their baby and make decisions about baptisms, burials and visitors with less time pressure, Agnitch said.
Before the CuddleCot, some families would have to send their baby down to the morgue for cooling, and then retrieve the baby for a short time during their hospital stay, Agnitch said.
“That is just like such a morbid experience,” Agnitch said. “It’s heartbreaking to know your baby’s down in the morgue.”
The CuddleCot allows grieving parents to keep their deceased infant at their bedside until they are ready to say goodbye, she said.
Although pregnancy loss and infant death are common, the topics are often stigmatized.
“I think there’s this taboo, or it’s too sad, or they don’t want to make other people feel uncomfortable,” Agnitch said. “We talk about death and the elderly, but it’s like we’re afraid to talk about it with infants.”
A future in labor and delivery
The experience with Greta changed Ashley Agnitch’s life.
She has since had another child, Jagger, who is 3, and the little brother to Dempsey, age 6. If Greta were alive today, she would be their middle child, turning 5 in April.
Shortly after her experience with Greta, Agnitch decided to change specialties and started working as a labor and delivery nurse. In July 2017, she left her job as a nurse at the Arroyo Grande Acute Rehabilitation Center to join the labor and delivery team at Marian Regional Medical Center in Santa Maria.
Last year, Agnitch transferred to the Stollmeyer Family Birthing Center at French Hospital to work with the same team that helped her through Greta’s birth and death.
“I thought it would be really hard to work where I had her, but instead, it’s actually really amazing to be with the people who got to meet her and care for her,” Agnitch said.

The experience of working with parents and newborns in labor and delivery, including some bereaved families, compelled Agnitch to give back to local families coping with infant loss.
“I think, as I became a labor nurse after having Greta ... it really took, like, me getting in there and working with these families and really gaining knowledge to see what a huge impact these CuddleCots could really have,” Agnitch said.
The memories, photographs and now the CuddleCot fundraising campaigns are just some of the ways the family honors their second-born daughter.
“If people ask me, ‘How many kids do you have?’ I say three,” Agnitch said. “And, depending on the situation, and I say, but we lost our second daughter to try Trisomy 18 shortly after birth. ... So that it opens up the opportunity where I hope that people feel open to talk to me about it.”
It seems she already has opened the door to more conversation about infant loss.
“I remember the death of our child, Elizabeth, only 12 hours old,” said GoFundMe donor D. Michael Perry. “It is hard to be a medical professional and loose (sic) a child — far harder than most people think. Thank you for sharing the story of your family and your loss.“
Donate to the CuddleCot GoFundMe page at gofund.me/68ab4763.
This story was originally published March 4, 2022 at 5:00 AM.